Navigating the World of Sedation: Understanding Its Types and Applications

Its time to get that dental work done and its going to hurt! The pain has to be dealt with and sedation is an option that can be considered. Sedation, a crucial component of many modern medical procedures, ensures patient comfort and facilitates the smooth execution of various treatments including dental work. Ranging from mild relaxation to deep sleep, sedation varies based on the procedure and patient needs. This comprehensive guide aims to elucidate the different types of sedation and their specific uses in the medical world.
Sedation is the process of using medication to relax, calm, or induce sleep in a patient during medical procedures. It helps manage pain and anxiety, ensuring patient comfort. The depth of sedation can range from minimal, where the patient remains awake but relaxed, to general anesthesia, where the patient is completely unconscious.
Types of Sedation
Minimal Sedation (Anxiolysis)
Minimal Sedation, commonly referred to as Anxiolysis, is the lightest level in the sedation spectrum. It's characterized by a state in which patients experience a reduction in anxiety (anxiolysis) with minimal effects on consciousness. Patients under minimal sedation remain awake and can understand and respond to verbal commands. Their cognitive function and coordination may be mildly impaired, but they retain the ability to maintain airway reflexes and breathe independently.
Administration and Medications
- Oral Sedatives: Often, minimal sedation is achieved using oral sedatives. Drugs like Diazepam are prescribed to be taken about an hour before the procedure. These medications help patients relax while remaining fully awake.
- Inhalation Sedatives: Nitrous oxide, also known as laughing gas, is a popular choice for minimal sedation. It’s administered through a mask and takes effect quickly, offering a rapid return to normalcy once the mask is removed.
- Topical Anesthetics: In some cases, topical anesthetics may be used in conjunction with oral or inhalation sedatives to numb the specific area being treated.
Common Uses
Minimal sedation is widely used in various medical and dental settings, particularly for patients who experience anxiety or fear about procedures. Common uses include:
- Dental Procedures: Such as cleaning or minor tooth extractions. It’s especially beneficial for patients with dental phobia.
- Diagnostic Procedures: For patients who feel anxious about undergoing MRI scans, CT scans, or other diagnostic imaging procedures.
- Dermatological Procedures: Like minor skin biopsies where patient cooperation is required.
Patients under minimal sedation often describe feeling relaxed and at ease, with a general sense of well-being. They remain conscious and can converse with the healthcare provider, but they may have limited memory of the procedure due to the amnesic effects of the sedatives.
Minimal sedation is an effective tool for managing anxiety and fear associated with medical procedures. Its ease of administration and quick recovery make it an excellent choice for many minor but anxiety-inducing procedures, greatly enhancing the patient experience without significant risks. As with any medical intervention, careful consideration of the patient's overall health and clear communication are key to ensuring a successful and comfortable procedure experience.
Moderate Sedation (Conscious Sedation)
Moderate Sedation, often termed Conscious Sedation, is a deeper form of sedation than minimal sedation but does not render the patient completely unconscious. It is designed to make patients feel more comfortable during a medical procedure while still allowing them to respond to verbal commands and physical stimulation. Unlike deeper sedation or general anesthesia, patients under moderate sedation maintain their own airway reflexes and breathing.
Administration and Medications
- Intravenous (IV) Sedatives: The most common method for administering moderate sedation is through IV, allowing for quick adjustment of medication levels. Drugs like Midazolam or Fentanyl are often used.
- Oral and Inhalation Options: In some cases, a combination of oral and inhalation methods might be used, though IV administration allows for more precise control of the sedation level.
- Combination Therapy: Often, a sedative is combined with an analgesic to minimize pain and discomfort during the procedure.
Common Uses
Moderate sedation is typically employed for procedures that require the patient to be relaxed but still responsive, such as:
- Endoscopic Procedures: Including colonoscopies and upper gastrointestinal endoscopies.
- Minor Surgical Procedures: Such as some types of outpatient surgery where deep sedation is not necessary.
- Dental Surgeries: Especially for patients with high levels of dental anxiety or for more complex dental procedures.
Patient experience during moderate sedation:
- Responsiveness: Patients can respond to verbal cues and physical stimulation, although their response might be slower.
- Awareness: They might have limited or no memory of the procedure due to the amnesic effects of the sedatives.
- Comfort: Patients generally feel relaxed and may drift in and out of a light sleep but can be easily awakened.
Moderate sedation is a valuable tool in various medical and dental settings, significantly enhancing patient comfort during procedures that might be too painful or anxiety-inducing under minimal sedation. The key to its success lies in the careful administration and monitoring of sedatives, ensuring a balance between patient comfort and safety. This level of sedation has greatly expanded the range of procedures that can be comfortably performed in a non-hospital setting, improving the overall patient experience in healthcare.
Deep Sedation
Deep Sedation represents a level of sedation deeper than conscious sedation but not as profound as general anesthesia. In this state, patients cannot be easily aroused but can respond to repeated or painful stimulation. Their ability to independently maintain ventilatory function may be impaired, and assistance in maintaining a patent airway could be required.
Administration and Medications
- Intravenous (IV) Administration: Deep sedation is commonly administered intravenously, allowing anesthesiologists or trained medical professionals to control the depth of sedation accurately.
- Medications Used: A combination of sedatives and analgesics, such as Propofol, Ketamine, or stronger opioids, are typically used. The specific agents chosen depend on the patient's medical history, the nature of the procedure, and the required sedation depth.
- Anesthesia Provider: Due to the deeper level of sedation, an anesthesia provider, such as an anesthesiologist or a nurse anesthetist, is usually required to administer the sedatives and monitor the patient.
Common Uses
Deep sedation is often utilized for procedures that require the patient to remain still for extended periods or for more invasive procedures, including:
- Certain Dental Procedures: Especially those involving oral surgery or for patients with severe dental anxiety.
- Pediatric Procedures: Used for children undergoing procedures who might not cooperate under lighter sedation levels.
- Minor Surgical Procedures: Such as some types of outpatient surgeries where general anesthesia is not necessary but patient movement needs to be minimized.
Patient Experience during deep sedation:
- Reduced Consciousness: Patients are in a state of near-unconsciousness and are unlikely to remember the procedure.
- Limited Responsiveness: They may only respond to repeated or painful stimuli.
- Assisted Breathing: In some cases, patients might require assistance with breathing, as their airway reflexes can be compromised.
Deep sedation is a critical tool in the arsenal of medical sedation, bridging the gap between conscious sedation and general anesthesia. It allows for a broader range of procedures to be performed with the patient in a state of deep relaxation and minimal awareness. However, it requires careful administration, vigilant monitoring, and specialized training, emphasizing patient safety and comfort. With these measures in place, deep sedation can significantly enhance the patient experience in various medical settings.
General Anesthesia
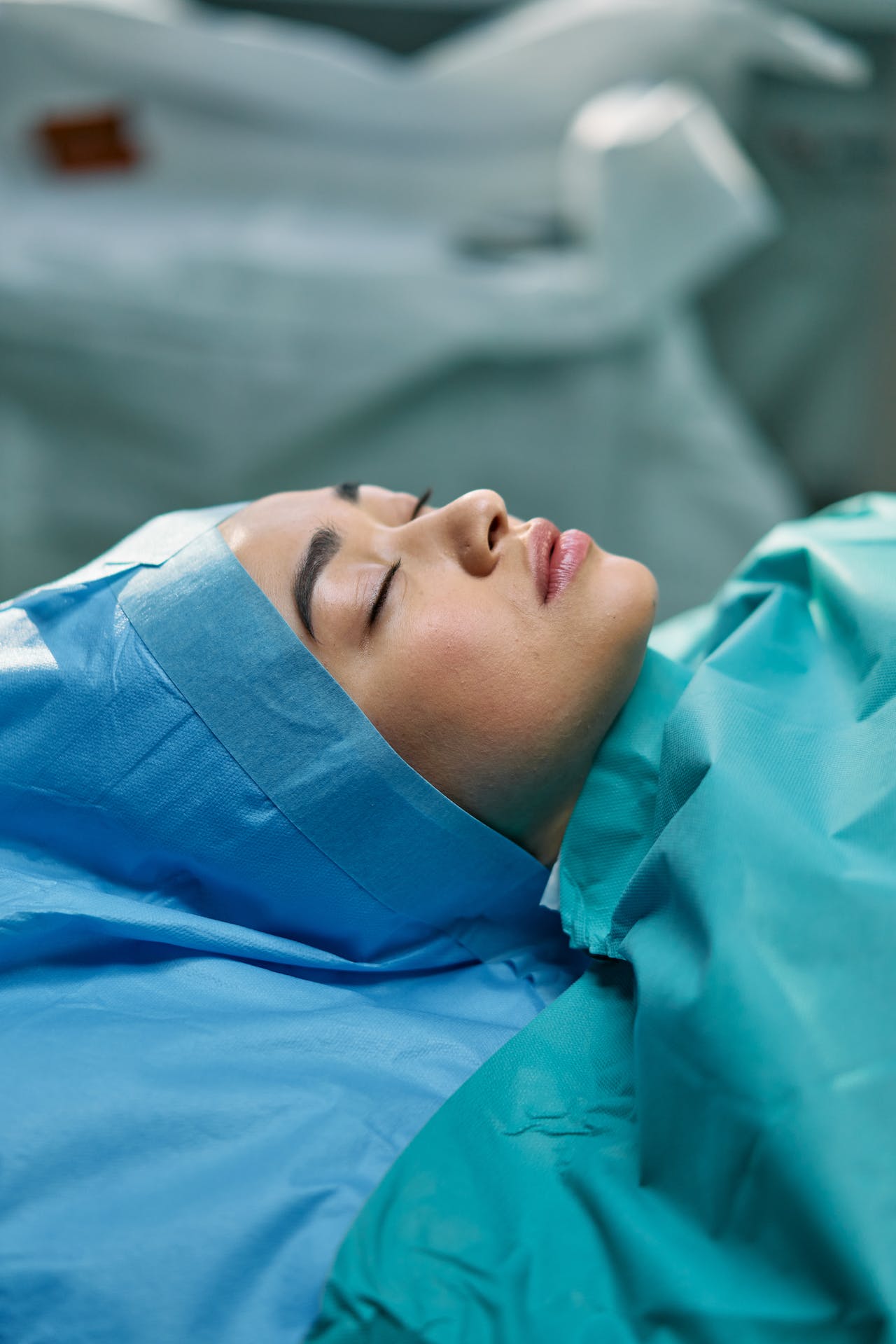
General Anesthesia represents the deepest level of sedation, wherein patients are rendered completely unconscious and have no awareness or sensation. Unlike other sedation forms, general anesthesia eliminates all sensations, including pain, and patients cannot be awakened until the effects of the anesthetic wear off or are reversed. It’s typically used for major surgeries and procedures where deep sedation is necessary.
Administration and Medications
- Intravenous and Inhalational Methods: General anesthesia is often initiated intravenously and maintained with inhaled anesthetics.
- Medications Used: A combination of medications, including sedatives, muscle relaxants, and pain relievers, are used. Common agents include Propofol, Sevoflurane, and Isoflurane, among others.
- Anesthesia Team: An anesthesiologist or a nurse anesthetist administers the anesthesia and monitors the patient throughout the procedure. This team is responsible for managing the patient’s vital functions during surgery.
Common Uses
General anesthesia is essential for:
- Major Surgical Procedures: Such as open-heart surgery, organ transplants, major joint replacements, and surgeries involving major organs.
- Procedures Requiring Immobility: Surgeries where patient movement could be life-threatening or could compromise the surgical outcome.
- Long or Complex Surgeries: Procedures that take a long time or are complex necessitate the use of general anesthesia.
Patient experience ynder general anesthesia:
- Unconsciousness: Patients have no awareness or memory of the procedure.
- No Sensation: All sensations, including pain, are completely blocked.
- Mechanical Ventilation: Patients often require assistance with breathing, as natural reflexes are inhibited.
General anesthesia is a critical component of modern medicine, enabling a wide range of complex and lengthy surgical procedures to be performed painlessly and safely. The administration of general anesthesia requires a specialized team of healthcare professionals to ensure patient safety and effective pain management. Advances in anesthetic drugs and monitoring technology continue to improve the safety and efficacy of general anesthesia, enhancing patient outcomes and recovery experiences.
Choosing the Right Type of Sedation
First and foremost, consult with your healthcare provider on the right options for you. The choice of sedation type depends on various factors, including:
- Procedure Type: The invasiveness and duration of the procedure are critical in determining the sedation level.
- Patient Health: Pre-existing medical conditions, allergies, and medication history can influence sedation choice.
- Patient Anxiety Level: Patients with significant anxiety may require deeper sedation for minor procedures.
Risks and Considerations
While sedation is generally safe when administered by trained professionals, it carries certain risks, such as:
- Allergic Reactions: Some patients may have allergies to sedatives.
- Respiratory and Cardiac Complications: Particularly with deeper levels of sedation.
- Post-Sedation Effects: Such as drowsiness, dizziness, and nausea.
Conclusion
Understanding the various types of sedation and their appropriate applications is essential for both healthcare providers and patients. With advancements in medical science, sedation methods have become safer and more efficient, allowing for a wide range of medical procedures to be performed with minimal discomfort. Whether it’s a simple dental cleaning or a complex surgical procedure, the appropriate use of sedation is key to patient comfort and procedural success.




